What does an Operating Department Practitioner (ODP) do?
There are three main aspects of the Operating Department Practitioner (ODP) role namely anaesthetics, surgery and post-anaesthetic care.
There are some overarching qualities that are necessary for any ODP. These include excellent communication skills including verbal, non-verbal and written. Treating patients with dignity and respect, maintaining confidentiality throughout.
Consider Edge Hill for your Operating Department Practitioner studies.
The anaesthetic ODP
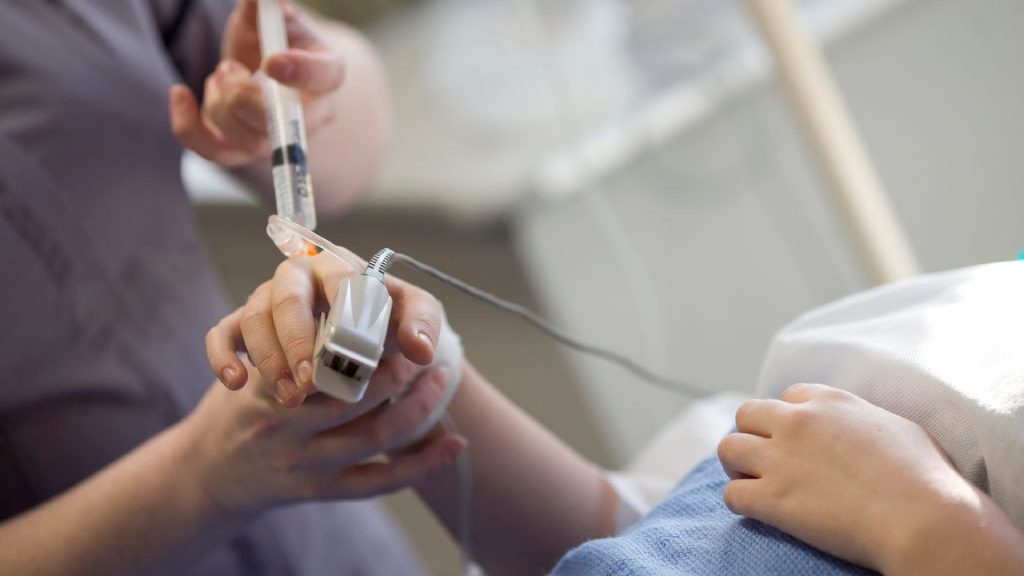
If you are working in the role of anaesthetic practitioner your day will start by ensuring that the environment and all equipment is safe and adequately prepared to accept the patient. This will include checking medical equipment like anaesthetic machines and vital signs monitors as well as ensuring that all equipment is clean and safe to use. Communication with all members of the theatre team is vitally important to ensure the safety of the patient and the team. The anaesthetic practitioner will discuss the planned care of the patient with the anaesthetist and prepare all the airway management and monitoring equipment that is necessary. Often the anaesthetic ODP is the first person that the patient meets and it is important to establish a good rapport with them from the outset. Once they are in the anaesthetic room they will apply vital signs monitoring to the patient and then assist the anaesthetist whilst they administer the anaesthetic type of choice. Once the patient is anaesthetised the ODP will ensure the patient is safely positioned on the operating table and that they are kept warm and secure throughout.
The scrub practitioner
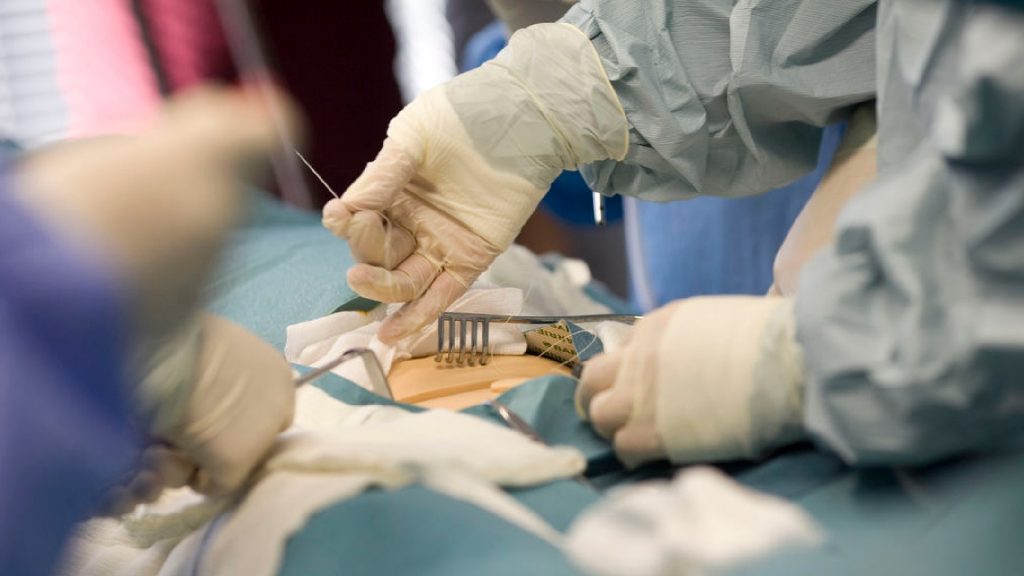
The theatre environment and equipment must be checked and its safety ensured. The scrub practitioner will support the surgeon who is carrying out the operation. They will have to wash their hands in a methodical manner (scrub) and put on a gown and gloves. They will have to ensure the availability and sterility of all equipment and ensure that it is accounted for at all times. Very often at this stage the patient is unconscious; therefore it is the scrub practitioners’ role to ensure that the patient remains safe throughout. This will include maintaining their dignity, ensuring confidentiality and treating them with respect. Surgery includes the role of the circulating practitioner. In this role the ODP will assist the Scrub ODP by passing any supplementary items as and when they are required by the surgeon. These items are passed in a way that maintains sterility and does not compromise patient care. At the end of the operation it is vitally important that a formal count of all instruments, swabs and needles is undertaken to ensure the safety of the patient.
The recovery practitioner
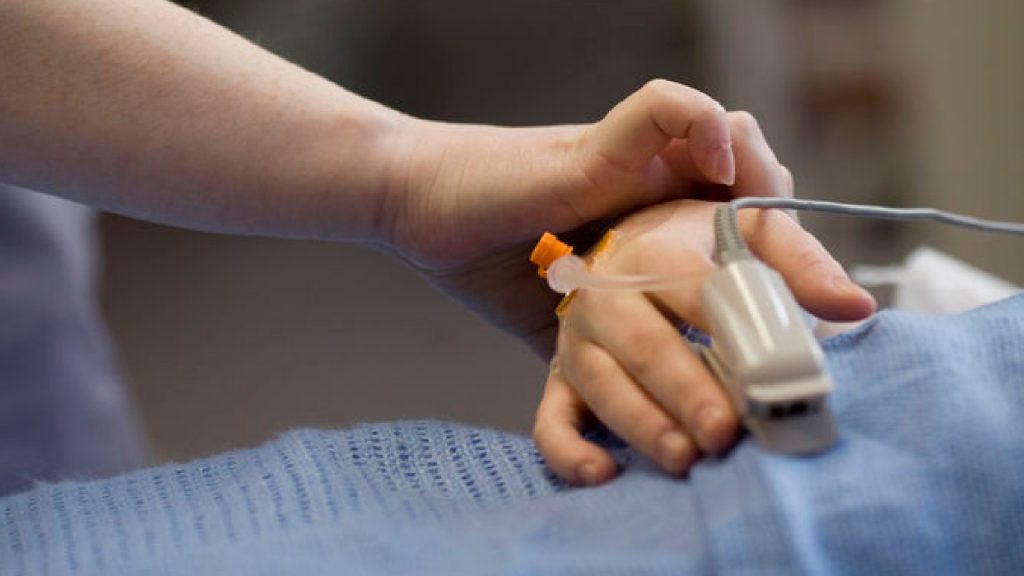
The recovery room will be prepared in the morning to ensure that it is clean and safe to accept patients and that all equipment is available and working, this will include all necessary emergency equipment. The recovery room is the area that the majority of patients will stay in for a minimum of 20 minutes post-operatively. The anaesthetist will hand over the care of the patient to the recovery practitioner detailing the care of the patient until that point including what operation they have had, drugs used and observations intraoperatively. Whilst receiving the hand over the recovery ODP will be ensuring the patient’s airway is safe and applying vital signs monitoring. Once the patient is breathing adequately and has satisfactory vital signs, the ODP will commence their documentation. Any deviation from the norm must be recognised early and acted upon immediately. Prior to the patient leaving recovery a certain criteria must be met. Once the ODP is satisfied that this criteria are met then the patient is then returned to the ward. The ODP will give a detailed handover of care to the ward staff who will continue to care for the patient throughout the remainder of their hospital stay.
How do the roles of an anaesthetic ODP, scrub practitioner, and recovery practitioner differ?
Anaesthetic ODP: The primary role of an anaesthetic ODP is to prepare the anaesthetic room and all the necessary equipment for the procedure. They also assist the anaesthetist in administering anaesthesia to the patient and ensure the patient’s safety during this stage.
Scrub practitioner: The scrub practitioner’s main responsibility is to assist the surgeon during the operation. This includes ensuring the sterility and availability of all surgical instruments and equipment, as well as accounting for all items used during the procedure.
Recovery practitioner: Recovery practitioners take care of the patient post-operation. They monitor vital signs, manage pain, and ensure the patient is ready to be moved back to the ward. The recovery room is typically where patients stay for a minimum of 20 minutes after surgery.
Is an Operating Department Practitioner the same as a nurse?
While both roles work in healthcare and share some similarities, they are distinct professions. ODPs are specifically trained to work in operating theatres and focus on providing care before, during, and after surgical procedures. Nurses have a broader scope of practice and can work in various healthcare settings, including hospitals, clinics, and community services.
Key responsibilities of an Operating Department Practitioner (ODP)
Operating Department Practitioners have varied roles depending on the specific area they work in. Here are the key responsibilities based on area.
In the anaesthetic phase
- Preparing the anaesthetic room and equipment.
- Performing pre-operative assessments and discussing care plans with the anaesthetist.
- Assisting the anaesthetist during the administration of anaesthesia.
- Ensuring the patient’s safety and well-being throughout the process.
During surgery:
- Preparing the operating theatre and surgical instruments.
- Ensuring sterility of the surgical environment.
- Assisting the surgeon by passing instruments in a timely and safe manner.
- Conducting a formal count of instruments and supplies to ensure nothing is left inside the patient.
In post-anaesthetic care
- Preparing the recovery room and making sure all essential equipment is available.
- Monitoring patient vital signs and overall condition upon arrival from surgery.
- Administering post-operative medications as directed.
- Ensuring a smooth handover of the patient back to ward care.
General responsibilities:
- Adhering to strict hygiene and safety protocols.
- Effective communication with the entire theatre team, including surgeons, nurses, and anaesthetists.
- Maintaining detailed patient records.
- Continual professional development through training and educational opportunities.
What qualifications do I need to become an Operating Department Practitioner (ODP)?
To become an ODP, you’ll typically need to complete a university degree in operating department practice. Entry requirements may vary but usually include A-levels or equivalent qualifications. Some universities may also require you to have experience in healthcare, which can be gained through volunteering or work placements.
Find out more about entry requirements for our BSc (Hons) Operating Department Practice course.
Salary
The typical salary for an Operating Department Practitioner (ODP) can vary widely based on factors like experience, location, and whether one is employed in the public or private sector.
In the UK in 2023*, newly qualified ODPs working for the NHS usually start at Band 5, with salaries ranging from approximately £25,000 to £31,000 per annum. As ODPs gain experience and take on more specialised roles, they can move into higher NHS Bands, such as Band 6 or 7, where salaries can range from around £31,000 to over £44,000 per annum.
Those in managerial or educational positions often earn more, sometimes exceeding £50,000 per year. Private sector salaries can be comparable or even more competitive, with additional benefits like bonuses or private health insurance sometimes offered.
Location also plays a role. For instance, ODPs working in London and the South East often earn higher salaries to compensate for the higher cost of living.
Additional earnings may also be possible through overtime, particularly for those working in critical care or specialised surgical units.
*For up-to-date salaries and pay scales, please visit NHS Employers.
What is the career progression like for an ODP?
Career progression for an ODP can vary depending on the individual’s goals and the opportunities available. Some ODPs choose to specialise in a particular area, such as paediatric anaesthesia or cardiac surgery, while others may move into managerial or educational roles. Additional qualifications and continuous professional development are key to career advancement.
Ready to start your journey as an Operating Department Practitioner?
f you’re considering a career as an Operating Department Practitioner, Edge Hill University offers a program that can provide you with the skills and knowledge you need for success in this field.